Q&A: How Technology Is Revolutionizing Care for Cleft and Craniofacial Differences
July 7, 2023
Cleft lip and cleft palate – when a baby’s lip or mouth doesn’t form completely during pregnancy – is the most common birth defect in the United States and puts one of every 600 newborns at risk for difficulty in feeding, language development, speech, hearing and dental health.
But new technological advances are poised to transform treatment and drastically improve patient outcomes.
Kazlin Mason, an assistant professor in the University of Virginia’s School of Education and Human Development, is a licensed speech language pathologist and director of the Imaging and Communication Outcomes Lab. In 2022, she received the American Cleft Palate/Craniofacial Association’s Emerging Leader award, given to an early-career professional who “exhibits exemplary accomplishment and dedication to the issues affecting people with cleft and craniofacial conditions.”In recognition of National Cleft and Craniofacial Awareness Month, we asked her about the latest technologies that are improving outcomes for children born with cleft and craniofacial differences.
This is because the velopharyngeal mechanism, or speech and resonance mechanism, is impacted by the cleft. This is an anatomic region at the back of our throat and it’s like a door between our nose and our mouth. The door is opening and closing for every speech sound that we say. It’s absolutely critical for clear and understandable speech. Speech pathologists are essential in helping to improve speech for these children, and this is a key area for research.
Q. What is your focus at the Imaging and Communication Outcomes Lab?
A. Our lab’s mission is to improve speech and surgical outcomes for individuals with cleft and craniofacial differences. We are integrating cutting-edge imaging technology along with 3D visualization and machine learning techniques. We’re also working to develop translational precision medicine approaches – moving things from the research lab into clinical practice – for assessment of speech function.
It’s very multidisciplinary work and heavily focused on the principles of team science, so we have a lot of collaborators. Here at UVA, we’re collaborating with colleagues in the Multiscale Muscle Mechanophysiology Lab to develop computational models of the velopharyngeal mechanism. We’re also working with surgeons in the UVA Cleft clinics, assessing outcomes and identifying anatomic predictors for success.
Our newest projects involve collaborations with radiologists, engineers and bioengineering students. We have clinical collaborators across the country as well.
Q. What are some of the existing problems or limitations affecting treatment?
A. In children with cleft palate, surgeries are often needed to improve the anatomy for speech, but many of these surgeries fail; speech doesn’t improve, or the outcome is worse than before surgery. That’s a huge burden on these patients.
Studies have shown that speech and surgical outcomes are better if the decisions are based on the patient’s individual anatomy. With current clinical methods, it can be challenging to get a clear, objective picture of an individual’s unique anatomy.
For example, a nasal endoscopy is a key imaging tool in craniofacial clinics. This is a video camera that goes up through the nose. So, in order to see a view of the anatomy, we’re sticking a video camera that’s the size of a spaghetti noodle up the nose of a young child and then asking them to say sounds and sentences. You can imagine how well that goes for most kids. It’s somewhat invasive and requires a lot of patient cooperation to actually see the anatomy, let alone analyze it.
Q. What are you currently working on in your lab to help solve those problems?
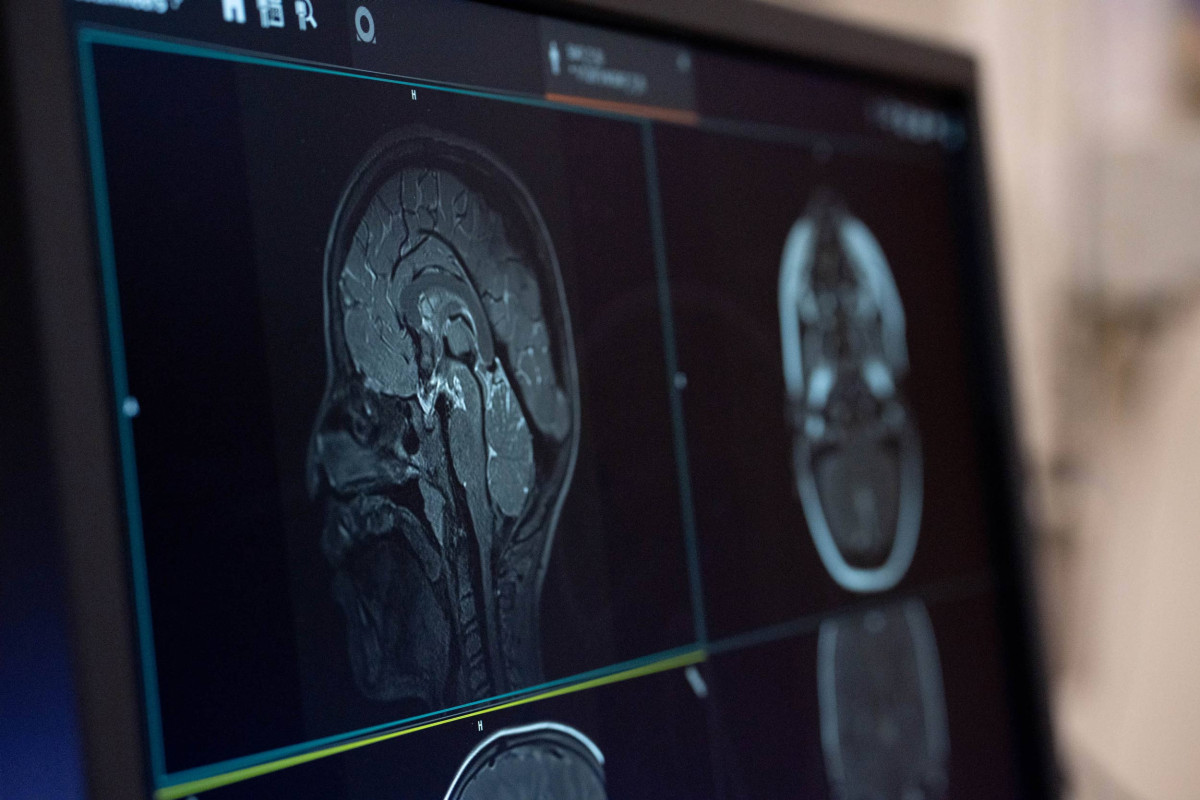
A. We’re doing a lot of exciting work with magnetic resonance imaging, or MRI, and new ways of analyzing data as a solution to current assessment gaps. We’re developing new clinical tools so that patients aren’t undergoing unnecessary procedures to get to that desired speech outcome.
One thing we’re focusing on is how to make it easier for clinicians to not only gather data using MRI, but also analyze that data. This is really important for complex cases where the cause of a speech problem is unknown, or prior attempts to repair have failed.
MRI has been around a long time, but for this population, it’s relatively new. That’s because typical scans can take hours and they often require patients to be sedated. But that’s not the case for our protocols.
In our area of work, we are focused on young children, and we need to acquire data while they are talking. So, our data collection is fast and kids are awake and participating in the imaging process. We prep the kids before scans and do everything we can to make it quick and fun. We have scan sequences that allow us to get speech data in 8 to 11 seconds, dynamic data in under two minutes, and some really detailed 3D anatomy scans in about 3½ minutes. We’ve been able to use this data to identify the best surgery for a patient and, through our collaborations with the School of Data Science and in Biomedical Engineering, we’re developing some pretty cool ways to analyze the data quickly, predict outcomes, generate reports and make it meaningful for a clinician.
Q. Any other interesting new advancements you see on the horizon?
A. Generative AI is such a buzzword right now, but I think applying AI algorithms to speed up data analysis – which we’re working on with the School of Data Science – will play a big role in moving the research forward, because we can analyze large anatomic datasets much more quickly.
You need so much data to generate accurate anatomic models for a normal craniofacial population. When you have an abnormal craniofacial anatomy – because it’s such a heterogeneous population – you just need to analyze volumes and volumes of data. Once we incorporate that data into these models and pipelines, I think we’re going to see an explosion in what can be done.
Q. How do you envision these advancements improving the process for patients?
A. With the rapid rate of technology advancements, I hope within the next few years we’re seeing MRI become a standard part of the clinical assessment process.
Ideally, a child would come in for their multidisciplinary team visit and all the providers would do their assessments, including an MRI scan. Then the team would deliberate and make a decision right then and there. It’s about streamlining the assessment process and getting good, objective data to inform the recommendations and, ultimately, reduce the number of surgeries needed to achieve normal speech function.
For our patients, that means more time in school, less of a financial and health burden, and an earlier foundation that’s going to set them up for successful communication across their lifespan.
Q. How can someone get involved with UVA’s work to advance treatments?
A. We have a number of studies that are currently in the recruitment phase. For anyone who has a cleft, parents of a child with a cleft, or providers working with children with cleft, we have active studies that they could participate in. There’s a participant interest and recruitment form on our lab website that we welcome anyone who may qualify for a study to fill out.
We also often take new students in the lab. If there are any UVA students interested in this area of research, they can always reach out to me. The Imaging and Communication Outcomes Lab supports students at the undergraduate, master’s and doctoral levels.